A thrombus is a blood clot that forms within a blood vessel. It can occur in both veins and arteries and can have serious health consequences if it blocks the flow of blood to vital organs. Some common causes of thrombus formation include injury to a blood vessel, slowed blood flow, and certain medical conditions such as heart disease and cancer. Treatment may include medications to dissolve the clot or surgery to remove it, as well as measures to prevent further clots from forming.
Mechanism of thrombus formation
The mechanism of thrombus formation involves a complex interplay of various factors. One of the key factors is the presence of a damaged or injured blood vessel wall. This damage can be caused by a variety of factors, including trauma, atherosclerosis, or inflammation. When the blood vessel wall is damaged, platelets (small blood cells involved in clotting) begin to stick to the damaged area and release chemicals that signal for more platelets to come and aggregate at the site of injury.
Simultaneously, the coagulation cascade, a series of chemical reactions in the blood, is activated to form a clot. Proteins in the blood called clotting factors work together to convert fibrinogen, a protein in the blood, into fibrin, which forms a mesh-like structure that traps red blood cells and platelets to form a clot.
Additionally, if blood flow is slow or stagnant, such as in a vein that is deep in the body, the platelets and clotting factors are more likely to aggregate and form a clot. Other factors that can contribute to thrombus formation include hypercoagulable states (abnormal blood clotting), certain medical conditions such as cancer, and certain medications that increase the risk of blood clots.
Treatment
Treatment for thrombus can vary depending on the location and severity of the clot, as well as the overall health of the patient. Some common treatments include:
- Anticoagulant medications: These medications, also known as blood thinners, are used to prevent the clot from getting larger and to reduce the risk of new clots forming. Common examples include heparin, warfarin, and newer oral anticoagulants such as dabigatran, rivaroxaban and apixaban.
- Thrombolytics: These medications, also known as clot busters, are used to dissolve the clot. They work by breaking down the fibrin that makes up the clot. Examples include tissue plasminogen activator (tPA) and urokinase.
- Thrombectomy: In some cases, a clot can be removed surgically through a procedure called thrombectomy. This is typically done for clots in larger blood vessels such as the legs or lungs.
- Interventional radiology: A catheter-based procedure can be used to break up or remove clots from blood vessels.
- Compression stockings: They are used to reduce the swelling and pain associated with a blood clot in the legs.
- Bed rest: for clots in legs, it is important to keep the affected limb elevated to reduce swelling and improve blood flow.
- Physical therapy: after the clot is treated and the patient is stable, physical therapy can help to improve circulation and prevent future clots.
It’s important to note that the treatment approach depends on the type and location of the clot, as well as the patient’s overall health. In some cases, a combination of treatments may be needed to effectively manage a thrombus.
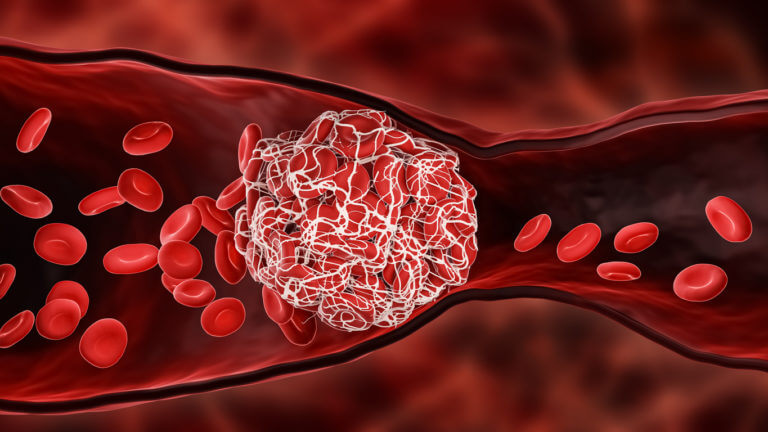
thrombus